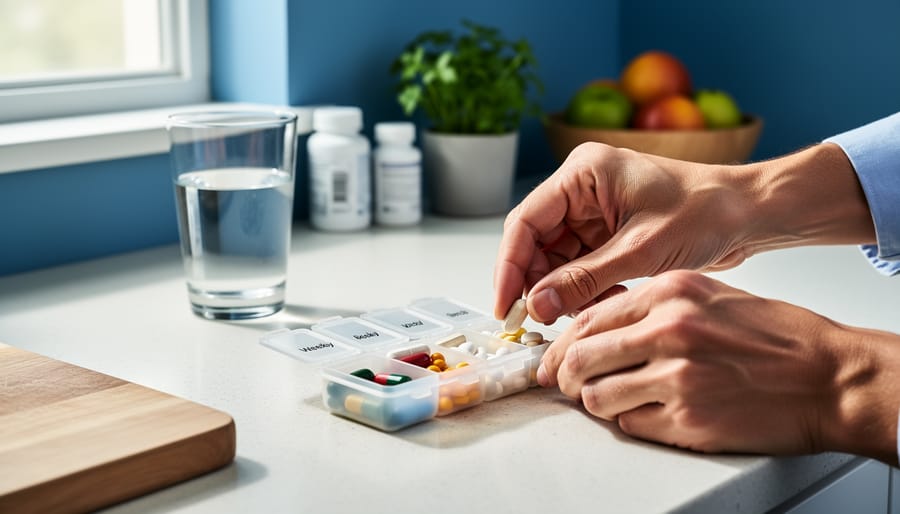
You take your medication faithfully for three days, then forget twice, then wonder if you really need it since you’re feeling fine. You know exercise helps your diabetes, yet your gym shoes gather dust. This isn’t weakness or laziness—it’s human nature, and it’s costing Canadian healthcare billions while quietly undermining your health goals.
Behavioral economics explains why smart, motivated people struggle with health decisions. Traditional healthcare assumes we make rational choices: doctors prescribe, patients comply. Reality is messier. We discount future benefits for immediate comfort, get overwhelmed by complex regimens, and fall victim to decision fatigue after long days. The gap between knowing what’s healthy and actually doing it isn’t about willpower—it’s about how our brains are wired.
Understanding these invisible forces changes everything. When you recognize that your brain naturally resists change, favors instant gratification, and relies on mental shortcuts, you can design systems that work with your psychology rather than against it. Small adjustments in how medications are packaged, how choices are presented, and how feedback is delivered can dramatically improve adherence without requiring superhuman discipline.
This science-backed approach transforms chronic disease management from an exhausting battle of willpower into strategic habit design. The strategies ahead aren’t theoretical—they’re proven techniques used by leading Canadian healthcare providers to help patients like you bridge the knowing-doing gap and achieve lasting health improvements.
What Behavioral Economics Reveals About Your Health Decisions
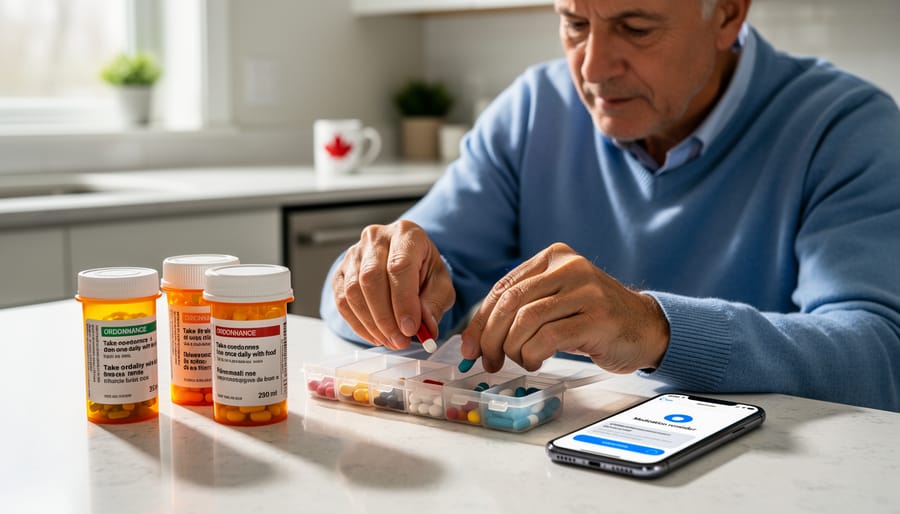
The Gap Between Knowing and Doing
Most Canadians with type 2 diabetes understand they should monitor blood sugar levels, exercise regularly, and follow dietary guidelines. Yet studies show that nearly half struggle to maintain these behaviours consistently. This disconnect between knowledge and action is called the intention-action gap, and it’s one of the most significant challenges in chronic disease management.
Consider Sarah, a 52-year-old from Ontario managing high blood pressure. She knows her medication schedule, understands the benefits of reducing sodium, and genuinely intends to walk daily. Despite this knowledge, she frequently skips her evening medication, orders takeout several times weekly, and her walking shoes gather dust. Sarah isn’t lazy or uninformed—she’s experiencing a predictable human phenomenon that behavioral economics helps explain.
The intention-action gap occurs because knowing what to do and actually doing it require different mental processes. Knowledge lives in our rational, planning brain, but behaviour happens in real-time when we’re tired, stressed, or distracted. When faced with immediate choices, our brains default to what’s easiest and most comfortable, even when we intellectually know better.
Research shows this gap widens when daily habits shape health outcomes over months and years rather than providing immediate results. Unlike touching a hot stove, which teaches instant consequences, skipping today’s medication or exercise produces no immediate discomfort—making it remarkably easy to postpone healthy choices indefinitely.

The Hidden Forces That Derail Your Chronic Disease Management
Present Bias: Why Tomorrow Always Seems Better
We often choose what feels good right now over what’s better for us later. This tendency, called present bias, explains why skipping today’s workout feels easier than imagining next year’s health complications, or why the immediate relief of avoiding an injection outweighs preventing future disease.
Present bias significantly impacts medication adherence and lifestyle changes. Research shows that approximately 50% of Canadians with chronic conditions don’t take medications as prescribed, often because the benefits feel distant while side effects or inconvenience are immediate. Similarly, we might skip physiotherapy exercises that could prevent pain months from now because we’d rather relax today.
This isn’t about willpower or laziness. Our brains are wired to value immediate rewards more heavily than future ones, even when we logically know the long-term choice is better. Understanding this can help you create strategies that work with your brain, not against it. Simple approaches like making healthy choices more convenient, connecting today’s actions to near-term benefits you care about, or using commitment devices can bridge the gap between knowing what’s good for you and actually doing it consistently.
Default Settings and the Power of Inertia
We’re creatures of habit, and our brains are wired to conserve energy by sticking with what’s familiar. This phenomenon, known as default bias or status quo bias, explains why many of us continue with our current treatment plans even when alternatives might work better. Research shows that people are significantly more likely to stay enrolled in programs, continue with medications, or maintain health behaviors when these become the automatic option rather than requiring active choice.
In healthcare, this inertia can work both for and against us. While it might keep someone from switching to a more effective medication, it can also be strategically designed to support positive behaviors. For example, automatic prescription refills increase medication adherence by removing the need to remember to reorder. Pre-scheduled follow-up appointments reduce the likelihood of missing important check-ins with your doctor.
The key insight for managing chronic conditions is recognizing that changing your default settings requires conscious effort. If your current routine isn’t serving your health goals, small adjustments to your environment can make healthier choices automatic, reducing the mental energy needed to maintain them consistently.
Loss Aversion: Why Setbacks Hit Harder Than Progress Feels Good
Have you ever noticed how one missed workout feels more demotivating than a week of consistent exercise feels encouraging? This is loss aversion in action—a core principle of behavioral economics showing that we feel losses about twice as intensely as equivalent gains. Research demonstrates this psychological tendency significantly impacts health behaviors, particularly in chronic disease management.
When you skip a single medication dose or break your exercise streak, the emotional impact often outweighs the satisfaction from previous successes. This disproportionate response can create a domino effect: one setback triggers feelings of failure, leading to abandoning healthy routines altogether. For Canadians managing conditions like diabetes or heart disease, this pattern becomes especially problematic because consistent, long-term adherence is essential.
Understanding loss aversion helps explain why small lapses derail progress. The solution isn’t avoiding setbacks entirely—that’s unrealistic—but rather reframing how you respond to them. Instead of viewing a missed dose as failure, recognize it as a single event in your ongoing health journey. Build recovery plans in advance: if you miss morning medication, take it as soon as you remember. Focus on your next healthy choice rather than dwelling on the misstep, which helps maintain momentum despite inevitable bumps along the way.
Choice Overload in Healthcare Decisions
When faced with multiple treatment options, medication schedules, or conflicting dietary advice, many Canadians experience decision paralysis that prevents them from taking any action at all. Research shows that having too many choices can actually decrease follow-through, particularly when managing chronic conditions like diabetes or heart disease.
For example, a patient presented with five different blood pressure medications, each with distinct side effects and scheding requirements, may feel overwhelmed and delay starting treatment altogether. Similarly, receiving numerous lifestyle recommendations simultaneously—change your diet, start exercising, improve sleep, reduce stress—often results in doing none of them.
Healthcare providers can reduce choice overload by prioritizing recommendations. Instead of presenting all possible options at once, focus on one or two key changes that will have the greatest impact. Breaking complex decisions into smaller, sequential steps makes them more manageable. Starting with simpler choices helps build confidence and momentum for more challenging decisions later.
Developing strong health literacy skills also empowers patients to evaluate options more effectively, reducing the anxiety that comes with complex healthcare decisions. When choices are simplified and properly explained, patients are more likely to take action and maintain their treatment plans.
Behavioral Economics Strategies That Actually Work
Make the Right Choice the Easy Choice
Our brains naturally choose the path of least resistance, so the key to better health habits is making healthy choices require less effort than unhealthy ones. This approach, called choice architecture, removes the need for constant willpower.
Start with smart defaults. When you pick up your prescription, ask your pharmacist to set up automatic refills. Research shows that people enrolled in automatic refill programs are 20-30% more likely to stay on their medications. Similarly, schedule your annual check-ups for the same month each year before leaving your doctor’s office.
Use visual cues and organizing tools strategically. A pill organizer placed beside your coffee maker links medication-taking to an existing habit. Pre-portion healthy snacks into grab-and-go containers at the front of your fridge, while moving less nutritious options to harder-to-reach spots.
Leverage technology to reduce friction. Set phone reminders for medications, or use apps that send adherence notifications. Many pharmacies now offer text alerts when prescriptions are ready, eliminating the extra step of checking in.
The goal is to design your environment so that the healthy choice becomes the automatic choice. When good behaviors require less thought and effort, you’re more likely to maintain them long-term, even when motivation fluctuates.
Use Commitment Devices to Your Advantage
Commitment devices are powerful tools that help you follow through on your health intentions by creating external accountability. These strategies work by making it harder to abandon your goals when motivation wavers.
One effective approach is pre-commitment: deciding your course of action before temptation strikes. For example, you might prepay for a series of physiotherapy sessions or schedule medical appointments months in advance. Research shows that people who prepay for health services are significantly more likely to attend.
Public accountability amplifies your commitment. Sharing your health goals with family, friends, or support groups creates social pressure to follow through. Consider joining a walking group or announcing your medication schedule to a trusted friend who can check in regularly.
Financial incentives tied to commitment can also drive behavior change. Some Canadian employers offer wellness program rewards for meeting health targets. You might also create personal stakes by contributing money to a goal-tracking app that donates to a cause you dislike if you fail to meet your commitments.
These strategies work because they shift the immediate consequences of your choices. Instead of distant health outcomes, you face immediate social or financial impacts, making it easier to stay on track with treatment plans even when motivation fades.
Reframe Your Goals to Avoid Loss
Research shows that people are more motivated to avoid losses than to pursue equivalent gains—a principle called loss aversion. You can harness this psychological tendency to strengthen your commitment to health goals.
Instead of focusing on what you’ll gain by taking your medication consistently, consider what you’ll lose if you don’t: your current level of independence, energy, or time with loved ones. This reframing often creates stronger motivation for behavior change.
Streak tracking is another powerful loss-aversion tool. When you’ve logged 30 consecutive days of taking your medication or checking your blood sugar, you become increasingly reluctant to break that streak. The longer your streak, the more you have to lose by missing a day. Use smartphone apps, wall calendars, or simple checkmark systems to visualize your progress.
Create what behavioral economists call “commitment devices”—small accountability measures that make it harder to abandon your goals. Share your medication schedule with a family member, set up automatic prescription refills, or join a support group where others track their progress alongside you.
The key is making your current progress visible and valuable. When you can see what you stand to lose, maintaining healthy behaviors becomes significantly easier than when you’re only focused on distant future benefits.
Simplify to Succeed
When managing chronic conditions like diabetes or heart disease, complex treatment plans can feel overwhelming. Behavioral economics shows that simplifying these regimens dramatically improves adherence and outcomes.
Start by breaking down your health goals into small, manageable steps. Instead of overhauling your entire lifestyle overnight, focus on one change at a time. For example, if you need to take multiple medications, establish a consistent routine by linking them to existing habits like morning coffee or brushing your teeth. This reduces decision fatigue and makes adherence automatic.
Healthcare providers can support this by prescribing combination pills when possible, reducing the number of daily decisions patients must make. Similarly, creating pre-planned meal guides or weekly exercise schedules eliminates the cognitive burden of choosing what to do each day.
Research from Canadian healthcare experts demonstrates that patients who follow structured routines show significantly better health outcomes. These simple lifestyle changes work because they align with how our brains naturally function.
The key is consistency over complexity. A simple plan you can follow beats a perfect plan that sits abandoned. By reducing choices and establishing clear routines, you free up mental energy to focus on what truly matters: your long-term health and wellbeing.
How Healthcare Providers Are Using These Insights
Canadian healthcare providers are increasingly putting behavioral economics into practice with impressive results. At several Ontario Family Health Teams, automatic prescription refill reminders sent via text message have boosted medication adherence rates by up to 25% among diabetes patients. These reminders use simple, friendly language and are timed strategically when patients are most likely to take action.
In British Columbia, some clinics have redesigned their appointment scheduling systems based on behavioral insights. By offering patients a choice between two specific appointment times rather than an open-ended “when works for you?” question, no-show rates have decreased significantly. This approach reduces decision paralysis and increases commitment.
Several Alberta diabetes clinics now use default options in their treatment plans. Instead of asking patients if they want to enroll in support programs, they automatically enroll them with an easy opt-out option. This subtle shift has tripled participation in diabetes education sessions.
The University Health Network in Toronto has integrated digital health tools that provide immediate feedback and small rewards for tracking blood pressure and glucose levels, tapping into our natural desire for instant gratification.
These practical applications demonstrate how patient-centered care approaches that acknowledge human psychology can make healthy behaviors easier and more automatic. The key is designing systems that work with our natural tendencies rather than against them, making the healthy choice the easiest choice.

Your Action Plan: Small Changes That Add Up
Ready to turn knowledge into action? Here’s your simple three-step plan to get started this week:
Step 1: Identify Your Biggest Barrier
Take five minutes to reflect on which behavioral hurdle affects you most. Are you forgetting to take medications? Struggling with healthy eating? Avoiding exercise? Write down the one behavior that, if changed, would make the biggest difference to your health.
Step 2: Choose One Strategy That Fits
Match your barrier to a behavioral economics solution:
For medication adherence: Set up automatic refills through your pharmacy and use a daily pill organizer with compartments. Place it next to your coffee maker or toothbrush as a visual cue.
For blood sugar management (diabetes): Pre-portion healthy snacks into grab-and-go containers every Sunday. Make the healthy choice the easy choice by keeping them at eye level in your fridge.
For physical activity: Commit to a specific time with a friend or family member. This social commitment makes it harder to back out than a promise to yourself.
For blood pressure monitoring: Link it to an existing habit. Check your blood pressure right after your morning coffee, using the same time daily.
Step 3: Track and Celebrate Small Wins
Use a simple calendar or app to mark each successful day. Research shows that seeing your progress builds momentum. After one week, you’ll have created the foundation for lasting change.
Remember, you’re not aiming for perfection. You’re building systems that work with your brain, not against it.
If you’ve struggled to stick with your medication schedule, track your blood sugar consistently, or maintain healthy habits despite your best intentions, you’re not facing a willpower problem—you’re facing a human problem. The science of behavioral economics shows us that our brains are wired with predictable biases and tendencies that make certain health behaviors genuinely difficult, regardless of how motivated we are.
The empowering news is that once you understand these natural human tendencies, you can design your environment and routines to work with them rather than constantly fighting against them. Simple changes like pre-portioning medications, setting up automatic appointment reminders, or reframing your health goals can remove invisible barriers that have been standing in your way.
Small behavioral tweaks compound over time into significant health improvements. You don’t need to overhaul your entire life overnight. Start with one evidence-based strategy that resonates with you, implement it consistently, and build from there. Managing a chronic condition is a marathon, not a sprint, and understanding the behavioral science behind your decisions gives you a powerful toolkit for sustainable success.