Understand that q4 neuro checks—short for “every four hours neurological checks”—are routine assessments healthcare teams perform to monitor your brain and nervous system function after injury, surgery, or during certain medical conditions. These brief evaluations typically take just a few minutes and involve simple tasks like following a moving finger with your eyes, squeezing the nurse’s hands with equal strength, answering orientation questions about the date and location, and having your pupils examined with a small light.
Expect your healthcare provider to ask you the same questions repeatedly throughout the day and night, which serves a vital purpose: detecting even subtle changes in your neurological status early, when intervention is most effective. This frequent monitoring represents evidence-based neurological care that has proven essential in identifying complications like increased brain pressure, bleeding, or stroke symptoms before they become critical.
Prepare for sleep interruptions during your hospital stay, as these four-hour intervals continue around the clock. While being woken at 2 a.m. and 6 a.m. may feel disruptive, this schedule isn’t arbitrary—research shows that neurological changes can occur rapidly and unpredictably, making consistent monitoring necessary for your safety.
Communicate openly with your care team about any new symptoms between scheduled checks, including headaches, vision changes, increased confusion, numbness, or weakness. Your observations matter significantly in building a complete picture of your neurological health and ensuring you receive timely, appropriate care.
Understanding Q4 Neuro Checks: The Basics
Who Needs Q4 Neuro Monitoring?
Q4 neuro monitoring is typically ordered for patients experiencing serious neurological conditions where brain function can change rapidly. Healthcare providers use these frequent checks to catch early warning signs of complications and respond quickly when needed.
Stroke patients often require Q4 neuro checks, especially in the first 24 to 72 hours after the event. During this critical window, brain swelling or bleeding can worsen, making close monitoring essential for preventing further damage.
Traumatic brain injury patients also need frequent neurological assessments. Even what appears to be a mild head injury can develop into a more serious condition, so regular checks help detect any deterioration early.
Patients recovering from brain or spine surgery typically undergo Q4 neuro monitoring as standard post-operative care. These checks ensure there’s no unexpected bleeding, swelling, or other complications affecting brain function.
Other conditions warranting frequent monitoring include brain tumors, seizures, meningitis, and increased pressure inside the skull. Your healthcare team will determine the appropriate monitoring schedule based on your specific situation and how stable your condition is. As your condition improves, the frequency of checks usually decreases.
The Science Behind Frequent Monitoring
Frequent neurological monitoring is grounded in solid medical evidence showing that early detection of changes can be life-saving. Research demonstrates that neurological conditions can deteriorate rapidly, sometimes within hours. By checking every four hours, healthcare teams can spot subtle warning signs before they become serious complications.
The human brain is remarkably sensitive to changes in blood flow, oxygen levels, and pressure. When something goes wrong, timing matters enormously. Studies show that catching issues like increased intracranial pressure, bleeding, or stroke progression in their early stages significantly improves patient outcomes and recovery potential.
Regular monitoring also helps prevent secondary complications. For example, detecting confusion or weakness early allows medical teams to intervene before problems like falls, aspiration, or further brain injury occur. This proactive approach reduces hospital stays and enhances long-term recovery prospects.
The Q4 schedule strikes an evidence-based balance between thorough surveillance and allowing patients adequate rest for healing. While it might feel disruptive, this monitoring rhythm has been validated through decades of neurological care research. Healthcare providers use this information to adjust treatments promptly, ensuring you or your loved one receives the most responsive, personalized care possible during a critical recovery period.
The Five Key Components Healthcare Providers Assess
Level of Consciousness
Level of consciousness is one of the most important indicators of brain function that healthcare providers assess during neurological checks. Your nurse will evaluate how alert and aware you are by observing your ability to respond to questions and follow simple commands. This assessment helps detect any changes in your neurological status early.
Healthcare teams often use the Glasgow Coma Scale, a standardized tool that evaluates three key areas: eye opening response, verbal communication, and motor function. You might be asked to open your eyes, answer questions like “What is your name?” or “Where are you?”, and follow commands such as “Squeeze my hands.” Each response receives a score, with higher scores indicating better consciousness levels.
Changes in alertness can signal important developments. If you become drowsier than expected, confused, or have difficulty staying awake, these shifts may indicate increased pressure in the brain, medication effects, or other neurological changes requiring prompt attention. Your healthcare team watches for these subtle changes to ensure timely intervention if needed. Understanding this process helps you know what to expect and why these frequent assessments matter for your recovery and safety.
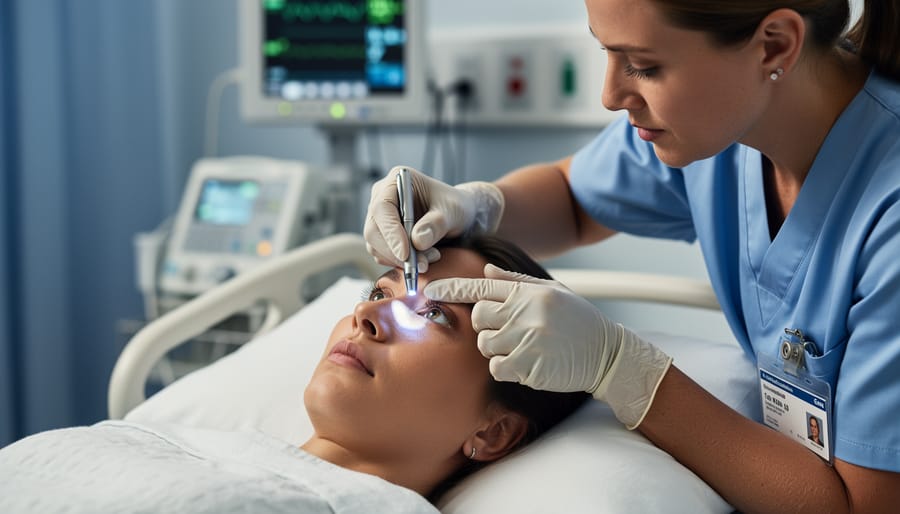
Pupil Response
Healthcare providers check your pupils to assess how your brain is functioning, as pupil response is controlled by specific nerves connected to your brain. During this check, a small light is shined into each eye to observe how your pupils react.
Normal pupils are equal in size and should quickly constrict (become smaller) when exposed to light, then dilate (enlarge) when the light is removed. Both pupils should respond together, even when light is only shined in one eye. This coordinated response indicates healthy brain function.
Abnormal findings include pupils that are unequal in size, don’t respond to light, react very slowly, or remain fixed in position. One pupil appearing larger than the other can signal increased pressure in the brain, while sluggish responses may indicate neurological changes requiring immediate attention.
Changes in pupil response help your healthcare team detect early signs of brain injury, stroke, or increased intracranial pressure. These observations are particularly important after head injuries or during recovery from neurological conditions. Monitoring pupils regularly allows medical professionals to intervene quickly if your condition changes, making this simple test a powerful tool for protecting your brain health.

Motor Function and Strength
Motor function and strength testing evaluates how well your brain communicates with your muscles. During this check, your healthcare provider will ask you to perform simple movements like squeezing their hands, pushing and pulling against resistance, or lifting your arms and legs. They’ll assess both sides of your body to compare strength and coordination.
This assessment is essential because the brain’s motor cortex controls all voluntary movements. Any weakness, especially if it appears suddenly or affects just one side of your body, can signal a neurological issue like a stroke, increased pressure in the brain, or nerve damage. For example, weakness on the left side of your body might indicate a problem in the right side of your brain.
Your provider will grade your strength on a standard scale, typically from 0 (no movement) to 5 (normal strength). They’ll also observe how smoothly you move and whether you can perform tasks like touching your nose with your finger, which tests coordination. These simple tests provide valuable information about your brain’s current function and help detect changes early when treatment is most effective.
Vital Signs
During q4 neuro checks, healthcare providers carefully monitor your vital signs because they offer important clues about how your brain and nervous system are functioning. Blood pressure is particularly significant, as sudden increases or decreases can indicate changes in pressure inside the skull or blood flow to the brain. Your heart rate provides insight into whether your body is experiencing stress or if certain brain areas that regulate heart rhythm are affected.
Breathing patterns are equally important during these assessments. Healthcare providers watch for changes in how fast or slow you breathe, as well as the depth and regularity of each breath. Abnormal breathing patterns can signal that specific parts of the brain responsible for controlling respiration may be impacted. These vital signs work together as a snapshot of your neurological health, helping medical teams detect potential complications early and respond quickly when needed. By understanding these connections, you can appreciate why nurses take these measurements so frequently and why each reading matters in your overall care plan.
Speech and Cognitive Function
Healthcare providers assess your cognitive function and speech to gain important insights into how your brain is working. During these checks, you’ll be asked simple questions like “What is today’s date?” or “Where are you right now?” to evaluate your orientation and memory. The nurse or doctor will listen carefully to how you speak, noting whether your words are clear or slurred, and if you can find the right words easily.
These assessments reveal crucial information about brain health. Clear, coherent speech suggests good coordination between the brain’s language centres and muscles. Difficulty speaking, confusion, or trouble understanding questions may indicate brain injury, stroke, or other neurological concerns requiring immediate attention.
You might also be asked to follow simple commands like “squeeze my hand” or “stick out your tongue.” These tasks help healthcare providers pinpoint which areas of the brain may be affected. Remember, these checks are quick, painless, and designed to catch potential problems early when treatment is most effective.
What Changes in Neuro Checks Mean for Treatment
Early Warning Signs That Prompt Action
Healthcare providers conducting Q4 neuro checks watch for specific changes that signal potential neurological complications. These warning signs include sudden difficulty speaking or understanding speech, noticeable weakness on one side of the body, changes in pupil size or response to light, increasing confusion or disorientation, severe headaches, and changes in breathing patterns.
When nurses or doctors notice these changes during routine checks, they act quickly. Time matters significantly in neurological conditions—early detection often means better outcomes and can prevent permanent damage. For example, if a stroke is caught within the first few hours, treatments are more effective at minimizing brain injury.
Your healthcare team uses a systematic approach, comparing current assessments with previous ones to spot even subtle changes. This careful monitoring allows them to intervene promptly, adjusting treatment plans or calling for additional specialists when needed. Understanding what providers are looking for helps you or your family members recognize why these frequent assessments are so important and how they directly contribute to protecting brain health and supporting recovery.
What to Expect If You or a Loved One Requires Q4 Neuro Checks
Tips for Supporting Recovery During Monitoring
If your loved one is undergoing q4 neuro checks, you play a valuable role in their recovery. First, help create a restful environment between assessments by minimizing noise and distractions. While frequent monitoring is necessary, your family member needs quality sleep for healing, so work with nurses to coordinate care activities when possible.
Communication with the healthcare team is essential. Don’t hesitate to ask questions about what specific changes they’re watching for or what the assessment results mean. Understanding medical terminology helps reduce anxiety and keeps everyone informed. Key questions to consider include: How long will q4 checks continue? What improvements are we hoping to see? When might monitoring frequency change?
Keep a simple notebook to track any concerns you notice between checks, such as confusion, unusual sleepiness, or changes in movement. Share these observations with nurses promptly. Remember that healthcare providers welcome your input since you know your loved one best.
Finally, take care of yourself too. Staying overnight in a hospital is exhausting. Step out for breaks, accept help from other family members, and maintain your own health so you can provide the best support during this critical monitoring period.
Understanding why you’re receiving Q4 neuro checks can bring peace of mind during what might feel like an overwhelming time. These regular assessments every four hours represent evidence-based neurological care designed to catch potential complications early when they’re most treatable. Canadian healthcare teams use standardized assessment tools that have been validated through extensive research to ensure your safety and recovery.
If you or a loved one are undergoing Q4 neuro checks, remember that this level of monitoring is actually a positive sign. It means your healthcare team is being thorough and proactive, following best practices in neurological care. While being awakened throughout the night might feel disruptive, these brief assessments provide critical information that guides your treatment plan and helps prevent serious complications.
Trust that your nurses and doctors are working together to provide you with quality, evidence-based care. The vigilant monitoring you’re experiencing reflects the high standards of Canadian healthcare, where patient safety comes first. Feel free to ask your care team questions about what they’re checking and why—they’re your partners in recovery and want you to feel informed and supported throughout your healing journey.

