Your bones are quietly losing density right now, and you might not realize it until a fracture happens. A bone density test, medically known as a DXA scan, is a quick, painless procedure that measures the strength of your bones and identifies osteoporosis before breaks occur. This 10-minute screening can literally prevent life-altering fractures, especially for women over 65 who face the highest risk.
Understanding when to get tested empowers you to take control of your bone health. Women should schedule their first bone density test at age 65, though earlier screening is recommended if you’ve experienced early menopause, have a family history of osteoporosis, take certain medications like corticosteroids, or have risk factors including low body weight or smoking. The test measures bone mineral density in your hip and spine, comparing your results to healthy young adults to determine your fracture risk.
Canadian healthcare covers bone density testing when medically indicated, making it accessible through your family doctor’s referral. Taking proactive steps today, including adequate calcium and vitamin D intake, regular weight-bearing exercise, and knowing your personal risk factors, protects your independence and quality of life for decades to come.
What Is a Bone Density Test?
How the Test Works
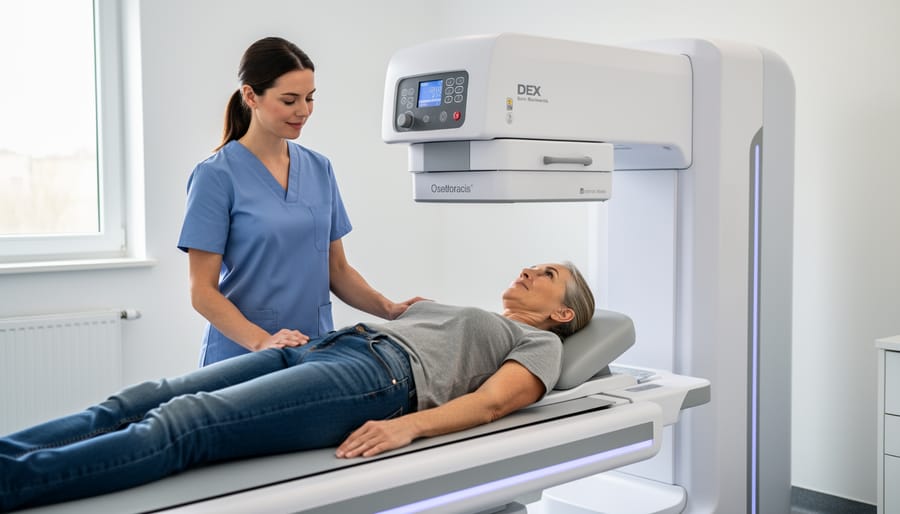
A bone density test, also called a DEXA scan (dual-energy X-ray absorptiometry), is a quick and painless procedure that measures the strength of your bones. You’ll lie comfortably on a padded table while a scanning arm passes over your body, typically focusing on your hip and lower spine, as these areas are most vulnerable to fractures. Some tests also scan your forearm.
The entire process takes just 10 to 20 minutes, and you can remain fully clothed as long as you avoid metal zippers, buttons, or jewelry near the scanning area. Unlike other imaging tests, you won’t need to enter a tunnel or confined space. The scanner uses very low levels of radiation—less than one-tenth of a standard chest X-ray—making it extremely safe.
During the scan, you’ll need to stay still while the machine takes measurements. There’s no discomfort involved, and you can return to your normal activities immediately afterward. Your healthcare provider will receive detailed results showing your bone mineral density compared to healthy young adults, helping determine your fracture risk and whether treatment is recommended.
Understanding Your Results
Your bone density test results are reported using two important scores. The T-score compares your bone density to that of a healthy 30-year-old woman, which represents peak bone mass. This is the primary score used to diagnose bone health conditions. A T-score of -1.0 or above is considered normal and indicates healthy bones. If your T-score falls between -1.0 and -2.5, you have osteopenia, meaning your bones are weaker than normal but not yet at the osteoporosis level. A T-score of -2.5 or lower indicates osteoporosis, which means your bones are significantly weakened and at higher risk for fractures.
The Z-score compares your bone density to other people of your same age, sex, and body size. This score is particularly useful if you’re premenopausal or under 50, as it helps identify if your bone density is unusual for your age group.
Understanding these numbers empowers you to take action. If your results show osteopenia or osteoporosis, don’t be discouraged. With proper treatment, lifestyle changes including weight-bearing exercise and calcium-rich nutrition, and regular monitoring, you can strengthen your bones and reduce fracture risk. Your healthcare provider will discuss personalized recommendations based on your specific results.
When Canadian Women Should Get Tested
Standard Age Recommendations
All Canadian women should have a bone density test at age 65 as part of routine age-appropriate health screenings. This baseline screening helps identify osteoporosis early when treatment is most effective.
If you’ve gone through menopause before age 45, talk to your doctor about testing earlier. Early menopause significantly impacts bone health due to reduced estrogen levels, which protect bones during reproductive years.
Women experiencing menopause should discuss their individual risk factors with their healthcare provider. Factors like family history of fractures, low body weight, smoking, or long-term steroid use may warrant earlier screening, sometimes as young as age 50.
The test, called a DXA scan, is painless and takes only 10 to 20 minutes. It measures bone mineral density in your spine and hips, the areas most vulnerable to fractures. Results guide your doctor in creating a personalized prevention or treatment plan to keep your bones strong and reduce fracture risk as you age.
Risk Factors That Mean Earlier Testing
While age 65 is the standard recommendation for bone density testing in Canada, certain risk factors mean you may benefit from earlier screening. Talk with your healthcare provider if any of these apply to you:
Family history plays a significant role—if your parent or sibling experienced a hip fracture or osteoporosis, your risk increases. Early menopause, whether natural or surgical, before age 45 reduces the time your bones benefit from protective estrogen.
Long-term use of certain medications can affect bone health, particularly corticosteroids taken for three months or more, some seizure medications, and certain cancer treatments. Your doctor can review your medication list to assess any concerns.
Several health conditions increase bone loss risk, including rheumatoid arthritis, celiac disease, inflammatory bowel disease, hyperthyroidism, and chronic kidney disease. Eating disorders, both past and present, can significantly impact bone density.
Lifestyle factors also matter. Low body weight (under 125 pounds or BMI below 19), smoking, excessive alcohol consumption, and prolonged periods of inactivity or immobility can all weaken bones over time.
If you identify with multiple risk factors, don’t wait—having an open conversation with your healthcare provider about earlier testing can help protect your bone health for years to come.
How Often to Retest
Retesting frequency depends on your initial results and risk factors. If your first bone density test shows normal results and you have no major risk factors, your doctor may recommend retesting every two to five years. Women with osteopenia (low bone density) typically need follow-up tests every one to two years to monitor changes. Those diagnosed with osteoporosis or taking bone-strengthening medications usually require annual testing to track treatment effectiveness.
Your healthcare provider will personalize your testing schedule based on factors like age, menopause status, medication use, and overall health. Canadian guidelines emphasize regular monitoring for women over 65 and younger women with increased fracture risk. If you experience significant health changes, such as starting corticosteroid therapy or experiencing a fracture, your doctor may adjust your testing timeline. Regular communication with your healthcare team ensures you receive timely retesting when needed.
Why Bone Density Matters for Women
The Estrogen Connection
Estrogen plays a vital role in maintaining strong, healthy bones by helping your body absorb calcium and supporting bone-building cells. During menopause, estrogen levels drop significantly, which accelerates bone loss. In the first five to seven years after menopause, women can lose up to 20 percent of their bone density, making this a critical window for bone health monitoring.
This dramatic shift in hormonal balance explains why women face four times the risk of osteoporosis compared to men. The decrease in estrogen affects your entire skeletal system, particularly impacting the spine, hips, and wrists. These areas become increasingly vulnerable to fractures as bone density declines.
Understanding this connection empowers you to take proactive steps. Regular bone density testing during and after menopause helps catch changes early, allowing you and your healthcare provider to develop an effective prevention or treatment plan before serious bone loss occurs.
The Real Cost of Weak Bones
Understanding the true impact of weak bones helps motivate preventive action. In Canada, one in three women will experience an osteoporosis-related fracture in their lifetime. These aren’t just minor injuries—hip fractures are particularly serious, with studies showing that 20% of people who break a hip face life-threatening complications within the first year.
Recovery from bone fractures presents significant challenges. Hip fractures often require surgery and months of rehabilitation. Many women find their mobility permanently affected, making everyday activities like grocery shopping, climbing stairs, or even walking to the mailbox difficult or impossible without assistance. This loss of independence can profoundly affect mental health and quality of life.
The ripple effects extend beyond physical limitations. Spinal fractures from osteoporosis can cause chronic pain, height loss, and a stooped posture that impacts breathing and digestion. Many women also experience anxiety about falling, leading them to avoid activities they once enjoyed.
The financial burden shouldn’t be overlooked either. Extended hospital stays, rehabilitation services, home modifications, and ongoing care create substantial costs for families and healthcare systems. However, the good news is that bone density testing identifies risks early, giving you time to take protective steps. Catching low bone density before fractures occur means you can maintain your active, independent lifestyle well into your later years.
How to Access Bone Density Testing in Canada
Getting a Referral
Starting a conversation about bone density testing with your doctor is straightforward. Simply express your interest during your next appointment, mentioning any risk factors like family history of osteoporosis, early menopause, or prolonged use of certain medications. Your healthcare provider will assess whether you meet the criteria for testing based on your age, medical history, and risk profile.
In Canada, you typically need a referral from your family doctor or nurse practitioner to access a bone density test covered by provincial health plans. The referral process is usually quick—your doctor will provide a requisition form that you’ll take to an approved imaging centre or hospital. Some provinces allow walk-in testing with a referral, while others require booking an appointment.
If you don’t have a family doctor, you can visit a walk-in clinic where a physician can assess your needs and provide a referral if appropriate. Be prepared to discuss your health history, current medications, and any concerns about bone health. Most referrals are processed within a few weeks, though wait times vary by location and facility availability.
Coverage and Costs
Coverage for bone density testing in Canada varies by province and depends on your risk factors and age. Most provincial health plans cover the test when you meet specific criteria, such as being over 65, having a fracture after age 40, or taking medications that affect bone health. If your doctor determines you’re at high risk for osteoporosis due to factors like early menopause, family history, or certain medical conditions, the test is typically covered.
Women under 65 without risk factors may need to pay out-of-pocket for bone density screening, with costs ranging from $75 to $200 depending on your location and the facility. Some private insurance plans include coverage for preventive bone density tests, so it’s worth checking your benefits.
To access a covered test, you’ll need a requisition from your healthcare provider. They’ll assess your risk factors and determine if testing is medically necessary. If you don’t meet provincial criteria but want peace of mind about your bone health, discuss options with your doctor. They can help you weigh the benefits of private testing against the cost and guide you toward the most appropriate timing for your situation.
Preparing for Your Test
Taking a few simple steps before your bone density test can help ensure accurate results and a smooth appointment. The good news is that minimal preparation is needed, making this an easy screening to fit into your schedule.
On the day of your test, wear comfortable, loose-fitting clothing without metal zippers, buttons, or underwire bras, as metal can interfere with the imaging. If your clothing contains metal, you may be asked to change into a hospital gown. Consider wearing athletic wear or cotton clothing with elastic waistbands for maximum comfort.
It’s important to avoid taking calcium supplements for at least 24 hours before your test, as calcium can create false readings on the scan. If you take prescription medications, continue those as normal unless your healthcare provider advises otherwise. You can eat and drink normally before your appointment.
Bring your health card and any relevant medical records, particularly if you’ve had previous bone density tests done elsewhere. Having those results for comparison helps your doctor track changes over time.
Come prepared with questions for your healthcare provider. Consider asking about your personal risk factors for osteoporosis, whether lifestyle changes could improve your bone health, and when you should schedule your next test. Write down your questions beforehand so you don’t forget them during your appointment.
Most bone density tests take only 10 to 30 minutes, making them convenient to schedule during your lunch break or between other appointments. This quick, painless screening provides valuable information about your bone health and future fracture risk.
What to Do After Your Test
Your healthcare provider will typically review your bone density test results with you at a follow-up appointment within a few weeks. The results are expressed as T-scores, which compare your bone density to that of a healthy 30-year-old adult. A T-score of -1.0 or above is considered normal, between -1.0 and -2.5 indicates low bone mass (osteopenia), and -2.5 or lower suggests osteoporosis.
If your results show normal bone density, your doctor will likely recommend retesting in two to five years, depending on your age and risk factors. Continue focusing on calcium-rich foods, vitamin D supplementation, weight-bearing exercise, and other healthy habits that support bone strength.
For results indicating osteopenia, your healthcare provider may suggest lifestyle modifications and possibly calcium and vitamin D supplements. They’ll want to monitor your bone health more closely with follow-up tests every one to two years.
If diagnosed with osteoporosis, don’t panic. Many effective treatments are available, including medications that can help strengthen bones and reduce fracture risk. Your doctor will create a personalized treatment plan and may refer you to a specialist. You’ll need regular monitoring to track your progress.
Feel concerned if you experience unexpected fractures, severe back pain, or loss of height between appointments. Contact your healthcare provider promptly with any worries. If you have questions about your results or women’s health questions in general, don’t hesitate to reach out to your medical team for clarification and support.
Building Stronger Bones at Any Age
Nutrition for Bone Health
Building strong bones starts with proper nutrition. Women need 1,000 mg of calcium daily before age 50, increasing to 1,200 mg after menopause. Excellent Canadian food sources include dairy products like milk, yogurt, and cheese, fortified plant-based alternatives, canned salmon with bones, sardines, and leafy greens such as kale and bok choy.
Vitamin D is equally important, helping your body absorb calcium effectively. Health Canada recommends 600 IU daily for adults under 70 and 800 IU for those older. During Canadian winters with limited sunlight, getting adequate vitamin D from food alone can be challenging. Good sources include fatty fish like salmon and mackerel, fortified milk and orange juice, and egg yolks.
Many Canadian women benefit from supplementation, particularly during winter months. Calcium supplements are available in various forms, with calcium citrate being easier to absorb for older adults. Combined calcium-vitamin D supplements offer convenience and ensure you’re getting both nutrients.
Consider consulting your healthcare provider about appropriate supplementation, especially if you have dietary restrictions or are at higher risk for osteoporosis. They can recommend the right dosage based on your individual needs and bone density results.


Exercise That Strengthens Bones
Building stronger bones requires regular physical activity that challenges your skeletal system. Two main types of exercise are particularly effective: weight-bearing activities and resistance training.
Weight-bearing exercises force you to work against gravity while staying upright. Walking, jogging, dancing, hiking, and climbing stairs are excellent options. Even a brisk 30-minute walk four times weekly can help maintain bone density. For those new to exercise, start with gentle walking and gradually increase your pace and duration.
Resistance training uses weights, bands, or your own body weight to strengthen both muscles and bones. Strength training exercises like squats, lunges, push-ups, and bicep curls stimulate bone formation when performed regularly. Beginners can start with light dumbbells or resistance bands, while more experienced individuals can progress to heavier weights.
Aim for at least 30 minutes of weight-bearing activity most days, combined with resistance training two to three times weekly. Activities like yoga and tai chi also support bone health by improving balance and reducing fall risk. Remember to consult your healthcare provider before starting any new exercise program, especially if you already have low bone density or other health concerns.
Lifestyle Changes That Protect Your Bones
Protecting your bone health involves adopting positive habits and avoiding those that weaken bones. If you smoke, quitting is one of the most important steps you can take. Smoking interferes with calcium absorption and reduces estrogen levels, both essential for strong bones. Limiting alcohol to no more than one drink per day also helps, as excessive consumption interferes with bone formation.
Fall prevention becomes increasingly important as bone density declines. Simple strategies include removing tripping hazards like loose rugs, installing grab bars in bathrooms, ensuring adequate lighting throughout your home, and wearing supportive footwear with non-slip soles. Regular balance exercises like tai chi or yoga can significantly reduce fall risk. Discussing any medications that cause dizziness with your healthcare provider is equally important. These practical changes, combined with regular bone density testing, create a comprehensive approach to maintaining skeletal health throughout your life.
Taking charge of your bone health is one of the most empowering steps you can take for your long-term wellness. Bone density testing isn’t something to fear—it’s a valuable tool that gives you important information about your body and helps you make informed decisions about your health journey.
If you’re a woman approaching menopause, have risk factors for osteoporosis, or simply want to understand your bone health better, having a conversation with your healthcare provider is an excellent first step. Don’t hesitate to ask questions about whether testing is right for you, what your results mean, and what actions you can take to strengthen your bones.
Remember that protecting your bone health extends beyond testing. Simple lifestyle choices like regular weight-bearing exercise, adequate calcium and vitamin D intake, and avoiding smoking all contribute to stronger bones throughout your life.
Your bones support you every day—now it’s time to support them. Schedule that appointment, ask those questions, and take an active role in maintaining your bone health. You deserve to move through life with strength and confidence at every age.

